|
8/12/2023 0 Comments Sleep related hypermotor epilepsy
Terminal remission (TR) as a function of (A) any underlying brain disorder (at least one of the following: intellectual disability, personal history of perinatal insult, pathologic neurologic examination, brain structural abnormalities): absence of any underlying brain disorder (green curve) and presence of any underlying brain disorder (blue curve) identified (B) typical sleep-related hypermotor epilepsy (SHE 100% of sleep-related events): patients with typical SHE (green curve) showed a higher TR rate than patients experiencing seizures in wakefulness (blue curve) (C) age at epilepsy onset: the cumulative probability of TR is higher in patients with age at onset ≥6 years (green curve) compared to patients with earlier epilepsy onset (blue curve) (D) combined vs single TR predictors (absence of any underlying brain disorder, typical SHE, and age at onset ≥6 years): the combination of at least 2 of the TR determinants identified (green curve) compared to having one or none of them (blue curve). on behalf of the American Academy of Neurology. Its outcome is primarily a function of the underlying etiology.Ĭopyright © 2016 The Author(s). 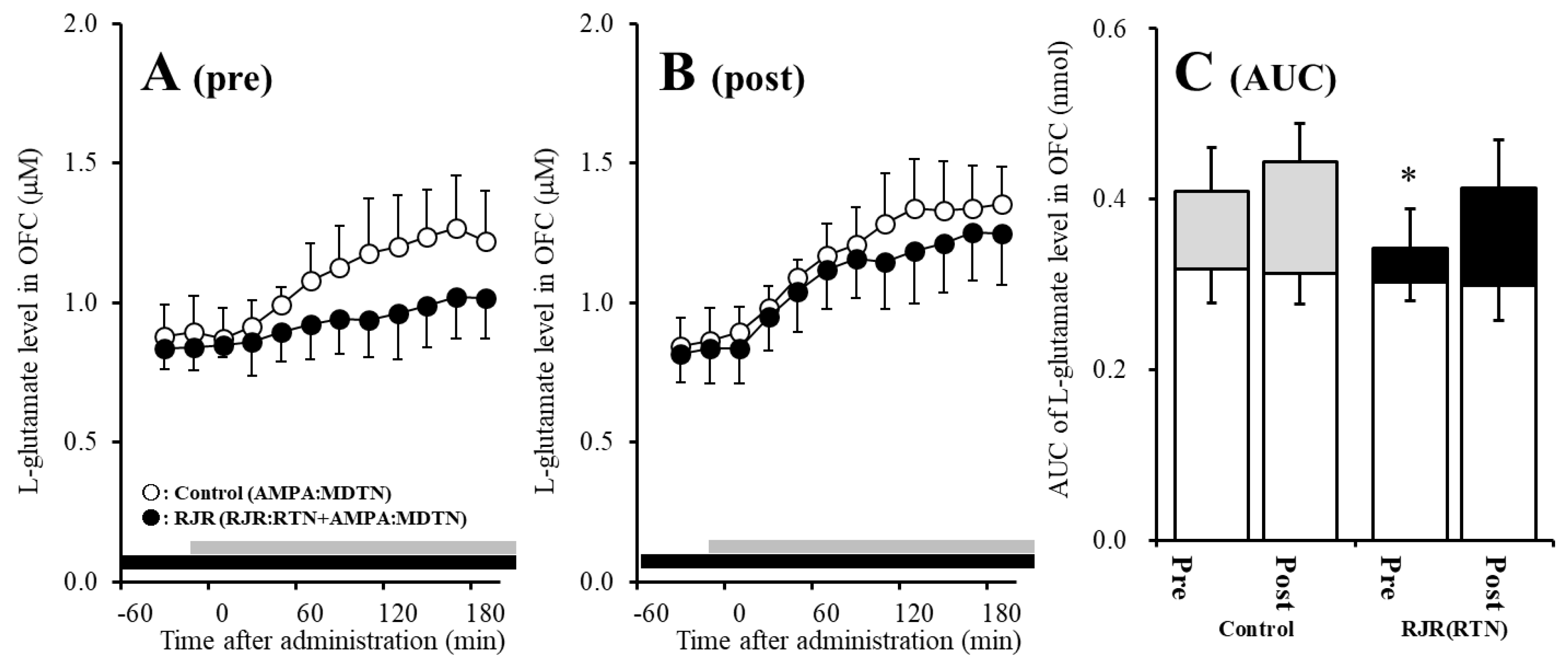
Our data show a poor prognosis of SHE after a long-term follow-up. Absence of any underlying brain disorder (hazard ratio 4.21, 95% confidence interval 1.26-14.05, p = 0.020) and typical SHE (hazard ratio 2.76, 95% confidence interval 1.31-5.85, p = 0.008) were associated with TR. At univariate analysis, any underlying brain disorder (any combination of intellectual disability, perinatal insult, pathologic neurologic examination, and brain structural abnormalities) and seizures in wakefulness were more frequent among the NTR group (p = 0.028 p = 0.043). The cumulative TR rate was 20.4%, 23.5%, and 28.4% by 10, 20, and 30 years from inclusion. At the last assessment, 31 patients achieved TR (TR group, 22.3%), while 108 (NTR group, 77.7%) still had seizures or had been in remission for <5 years. Forty-five percent of patients had at least 1 seizure in wakefulness lifetime and 55% had seizures only in sleep (typical SHE). SHE was sporadic in 86% of cases and familial in 14% 16% of patients had underlying brain abnormalities. We included 139 patients with a 16-year median follow-up (2,414 person-years). Univariate and multivariate Cox regression analyses were performed. Major points of agreement emerged on: (i) the relationship of the seizures with sleep and not with the circadian pattern of seizure occurrence (ii) the possible extrafrontal origin of hypermotor seizures, without substantial differences in seizure semiology. We used Kaplan-Meier estimates to calculate the cumulative time-dependent probability of TR and to generate survival curves. 
Terminal remission (TR) was defined as a period of ≥5 consecutive years of seizure freedom at the last follow-up. We retrospectively reconstructed a representative cohort of patients diagnosed with SHE according to international diagnostic criteria, sleep-related seizures ≥75% and follow-up ≥5 years. To assess the long-term outcome of sleep-related hypermotor epilepsy (SHE).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
